

Have you ever wondered what happens behind the scenes after your doctor visit? Medical billers are the unsung heroes who ensure healthcare providers get paid accurately and on time. Understanding their daily workflow can help you appreciate the complexity of healthcare billing and why choosing the right billing partner matters for your practice.
What Does a Medical Biller Actually Do?
A medical biller serves as the financial backbone of any healthcare practice. These professionals translate healthcare services into billable claims, submit them to insurance companies, and ensure providers receive proper reimbursement. Think of them as financial detectives who navigate the complex world of insurance claims, medical codes, and payment processing.
Every morning, a medical biller starts their day reviewing pending tasks, checking emails for insurance responses, and preparing for the workflow ahead. Their role combines attention to detail, problem solving skills, and constant communication with insurance companies, patients, and healthcare providers.
Morning Routine: Setting the Foundation
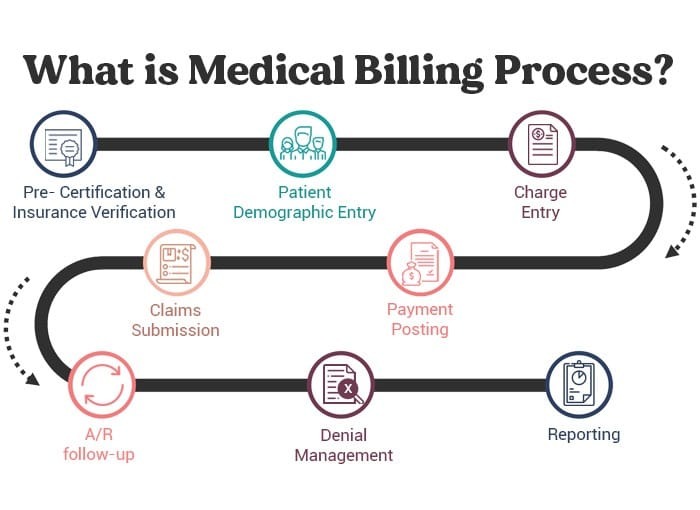
Patient Registration and Insurance Verification
The day typically begins between 8am and 9am with reviewing patient appointments scheduled for the day. Medical billers verify insurance eligibility before patients arrive, checking coverage limits, copayments, deductibles, and authorization requirements. This critical step prevents claim denials and ensures smooth payment processing.
Insurance verification involves contacting insurance providers through online portals or phone calls to confirm active coverage. Without accurate verification, practices risk submitting claims that will be rejected, delaying revenue and creating additional work. Professional medical billing services in Florida specialize in streamlining this process to maximize efficiency.
Reviewing Medical Codes and Documentation
After medical coders assign diagnosis and procedure codes using ICD-10 and CPT coding systems, billers carefully review this documentation. They ensure codes accurately reflect the services provided and match the supporting medical records. Any discrepancies must be corrected immediately to avoid claim rejections.
This review process requires deep knowledge of medical terminology, coding standards, and insurance requirements. Experienced billers can quickly spot potential issues that might trigger denials, saving valuable time and preventing revenue loss.
Midday Tasks: Claim Submission and Follow Up

Preparing and Submitting Claims
Medical billers spend significant time preparing claims for submission to insurance companies. They compile patient demographics, insurance information, medical codes, and provider details into standardized claim forms. Most submissions happen electronically through clearinghouses, which scrub claims for errors before forwarding them to payers.
The claim submission process requires meticulous attention to detail. A single error in patient date of birth, insurance policy number, or procedure code can result in claim denial. Quality medical billing companies in Florida use advanced software systems that automatically check for common errors before submission, reducing rejection rates.
Accounts Receivable Management
Throughout the day, billers monitor accounts receivable reports to track outstanding claims. They follow up on unpaid claims that have been pending for 30, 60, or 90 days. This involves calling insurance companies, checking claim status, and investigating reasons for payment delays.
Effective AR management is crucial for maintaining healthy cash flow. Billers must be persistent yet professional when communicating with insurance representatives, often navigating complex phone systems and explaining claim details to expedite payment.
Afternoon Activities: Denial Management and Patient Communication
Handling Claim Denials and Appeals
One of the most challenging aspects of medical billing is managing denied claims. Billers review denial reasons, which might include coding errors, missing documentation, lack of medical necessity, or authorization issues. They determine whether claims can be corrected and resubmitted or require formal appeals.
Specialized billing services like cardiology medical billing companies understand specialty specific denial patterns and have expertise in overturning rejections. The appeals process involves writing detailed letters, gathering supporting documentation, and meeting strict deadlines.
Payment Posting and Reconciliation
When payments arrive from insurance companies, billers post them to patient accounts, carefully matching remittance advice with expected amounts. They identify underpayments, apply contractual adjustments, and determine patient responsibility for remaining balances.
This reconciliation process ensures accurate financial records and identifies when insurance companies have not paid according to contracted rates. Billers may need to contact payers to dispute incorrect payments and request adjustments.
Patient Billing and Collections
After insurance processing, billers generate patient statements for outstanding balances including copays, deductibles, and non covered services. They answer patient questions about bills, explain insurance benefits, and establish payment plans when needed.
Professional communication is essential during collection activities. Billers must balance the need to collect payments with maintaining positive patient relationships. Services like Credentialing billing services ensure providers are properly enrolled with insurance networks to minimize patient out of pocket expenses.
Supporting Specialized Practices
Different medical specialties have unique billing requirements. Dental Billing services handle coordination of benefits and dental specific codes, while orthopedic billing services in Florida manage complex surgical procedures and durable medical equipment claims.
Comprehensive revenue cycle management services in florida address every aspect of the billing process, from patient registration through final payment, optimizing financial performance for healthcare practices.
End of Day: Reporting and Planning
Before closing, medical billers review productivity metrics, update task lists, and prepare reports showing daily collections, pending claims, and denial rates. They communicate with practice managers about financial trends and potential revenue concerns.
This analytical work helps practices make informed business decisions and identify areas for improvement in their billing operations. Modern billing software provides dashboards showing key performance indicators that guide strategic planning.
Conclusion: Why Professional Medical Billing Matters
The daily life of a medical biller involves juggling multiple responsibilities, solving complex problems, and maintaining detailed financial records. Their work directly impacts practice revenue, compliance, and patient satisfaction.
Many healthcare providers choose to outsource these critical functions to experienced professionals who have the expertise, technology, and resources to maximize reimbursement. If you are looking for reliable medical billing support, visit ACP Billing Services to discover how expert billing management can transform your practice revenue and allow you to focus on what matters most: providing excellent patient care.
Frequently Asked Questions
What qualifications does a medical biller need?
Medical billers typically need certification in medical billing and coding, knowledge of healthcare regulations, proficiency with billing software, and excellent attention to detail. Many hold credentials from organizations like AAPC or AHIMA and have completed specialized training programs.
How much can medical billers increase practice revenue?
Professional medical billing services can increase practice revenue by up to 20 percent through improved claim accuracy, faster submission times, reduced denials, and effective AR management. They also reduce administrative costs and allow healthcare providers to see more patients.
What is the biggest challenge medical billers face daily?
The biggest challenges include managing claim denials, staying current with constantly changing insurance requirements, handling high volumes of claims accurately, and maintaining compliance with healthcare regulations like HIPAA while ensuring timely reimbursement.





