
Are you losing thousands of dollars each month due to denied claims? You are not alone. Healthcare practices across the United States face a growing challenge that directly impacts their financial stability. Every denied claim represents more than just delayed payment. It means additional staff time, administrative burden, and potential revenue loss that can cripple your practice cash flow.
Research shows a sobering reality. Nearly 85% of claim denials are preventable, yet 65% are never reworked or appealed. Why? Most practices lack the time, expertise, or systematic approach to tackle this costly problem. The average denial costs between $25 to $117 to rework, and when denials pile up, these expenses quickly multiply into tens of thousands in lost revenue annually.
This comprehensive guide reveals 20 proven claim denial management solutions that successful healthcare practices use to maintain healthy cash flow. Whether you run a small clinic or multi-specialty practice, these strategies will help you prevent denials before they happen, resolve them quickly when they occur, and build a sustainable system that protects your revenue.
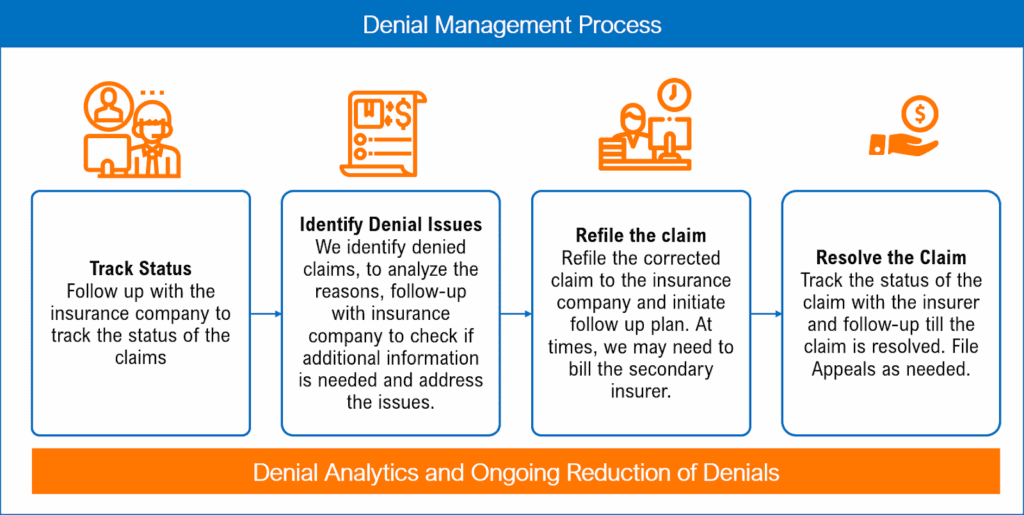
Understanding Why Claim Denials Hurt Your Bottom Line
Before diving into solutions, you need to understand the real cost of denial management. When insurance payers deny your claims, the financial impact extends far beyond the claim amount itself. Your staff spends valuable hours investigating the denial reason, gathering documentation, correcting errors, and resubmitting appeals. During this time, your accounts receivable age, collection rates drop, and your practice absorbs operational costs without corresponding revenue.
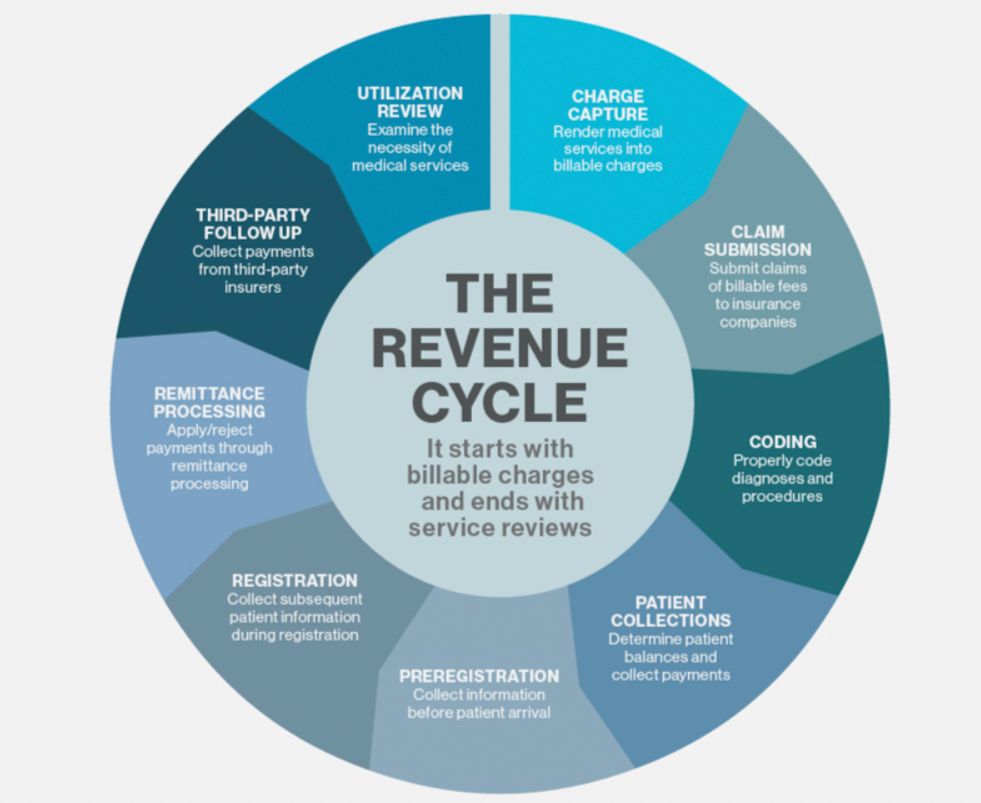
The healthcare revenue cycle functions like a carefully balanced ecosystem. When denials disrupt this flow, they create ripples throughout your entire billing operation. Clean claims that pass through on first submission generate steady cash flow. Denied claims, however, require rework that diverts resources from new patient services and creates backlogs that compound over time.
The 20 Most Effective Claim Denial Management Solutions
Eligibility and Authorization Issues
Solution 1: Implement Real Time Eligibility Verification
Verify patient insurance eligibility before every appointment, not just at initial registration. Insurance coverage changes frequently due to employment changes, policy modifications, or benefit year resets. Use automated eligibility verification tools that check coverage in real time and flag inactive policies before services are rendered. This proactive approach prevents the most common denial reason and ensures you only provide services to patients with active coverage.
Solution 2: Master Prior Authorization Requirements
Create a comprehensive prior authorization tracking system that identifies which procedures require approval from each payer. Submit authorization requests as soon as you schedule procedures that need approval, giving payers adequate time to review and respond. Document all authorization numbers accurately and include them on every claim submission. Missing prior authorization represents one of the easiest denials to prevent with proper planning.
Solution 3: Verify In Network Provider Status
Confirm that all providers rendering services are properly credentialed and enrolled with relevant insurance plans. Track credentialing expiration dates and submit renewal applications at least 90 days before expiration. When providers are not in network, obtain written acknowledgment from patients regarding their financial responsibility before delivering care. This prevents surprise denials and protects both your practice and your patients.
Solution 4: Double Check Patient Demographics
Train front desk staff to verify every detail on insurance cards at each visit. Even a single transposed digit in the policy number, incorrect date of birth, or misspelled name will trigger an automatic denial. Create a checklist that staff must complete during check in, and photocopy both sides of every insurance card. The back contains critical claims filing addresses and coordination of benefits information that billing staff need for accurate submission.
Solution 5: Confirm Benefit Limits Before Service
Many insurance plans limit the number of visits or specific services covered within a calendar year. Before scheduling appointments, check remaining benefits to ensure coverage is available. When patients exhaust their benefits, inform them in advance and collect payment at the time of service. This transparency prevents denials and protects your practice from uncompensated care.
Documentation and Coding Excellence
Solution 6: Document Chief Complaints Thoroughly
Every patient encounter must include a clear, concise chief complaint that explains why the patient sought care. Vague or missing chief complaints lead to denials based on incorrect levels of care or medical necessity questions. Train providers to document specific symptoms, duration, and severity that justify the services billed. Strong documentation supports your claims during audits and appeals.
Solution 7: Code to Highest Specificity Level
Medical coding has become increasingly detailed with ICD 10 requiring specificity that earlier coding systems did not demand. Use codes that describe the exact condition, laterality, encounter type, and other details that modern coding requires. Unspecified codes trigger payer scrutiny and often result in denials or downgrades that reduce your reimbursement.
Solution 8: Master Modifier Usage
Understand when and how to apply modifiers correctly to your procedure codes. Modifier 25, one of the most commonly used yet frequently misapplied modifiers, requires a significantly separate and identifiable evaluation and management service on the same day as a procedure. Incorrect modifier usage generates denials that could have been avoided with proper education and claim review.
Solution 9: Understand Bundling Rules
Familiarize your coding team with National Correct Coding Initiative edits and payer specific bundling policies. Some procedures cannot be billed separately because payers consider them included in other services. Attempting to unbundle services that should be reported together results in denials and potential compliance issues. Invest in coding software that applies these edits before claim submission.
Solution 10: Match Place of Service Codes Correctly
Ensure the place of service code on your claim matches where you actually delivered the service. Common mistakes include using office codes for hospital services or vice versa. Each place of service code has specific billing rules and reimbursement rates, so accuracy is essential for clean claims and proper payment.
Claim Submission Best Practices
Solution 11: Establish Claim Scrubbing Protocols
Implement automated claim scrubbing technology that reviews every claim before submission. These tools identify missing information, coding errors, and payer specific requirements that would trigger denials. By catching mistakes before claims leave your office, you dramatically increase your first pass acceptance rate and reduce rework costs.
Solution 12: Include All Required Documentation
Attach supporting documentation when payer policies require it with initial claim submission. Medical records, operative reports, authorization letters, and other supporting documents should accompany claims that payers typically review for medical necessity. Submitting complete claims upfront accelerates processing and prevents unnecessary denials for additional information requests.
Solution 13: Verify Referral Information
When treating referred patients, confirm you have accurate referral numbers and referring provider information before submitting claims. Payers deny claims with missing or incorrect referral data to ensure care coordination and adherence to managed care requirements. This simple verification step prevents easily avoidable denials.
Solution 14: Submit Claims Within Filing Deadlines
Every insurance carrier establishes specific timeframes for claim submission, typically ranging from 30 to 365 days from date of service. Track these deadlines carefully and prioritize claim submission to ensure you file within allowed timeframes. Untimely filing denials are often non appealable, making these losses permanent and preventable with better workflow management.
Solution 15: Include National Drug Code When Required
For claims involving medications, injections, or certain supplies, include the National Drug Code identifier when payer policies require it. This unique identifier provides essential details about the specific medication administered and ensures accurate reimbursement. Missing NDC information generates denials that delay payment unnecessarily.
Denial Resolution and Prevention Systems
Solution 16: Build a Denial Tracking Database
Create a comprehensive system that captures every denial your practice receives. Track the denial reason, payer, provider, service type, and resolution outcome. Analyze this data regularly to identify patterns and trends that reveal systemic problems. Understanding your specific denial profile allows you to target interventions where they will have the greatest impact.
Solution 17: Prioritize Denials by Financial Value
Not all denials deserve equal attention given limited staff resources. Categorize denials by dollar amount and likelihood of successful appeal. Focus your efforts on high value denials with strong appeal potential first, then work through smaller denials as time permits. This strategic approach maximizes revenue recovery with available resources.
Solution 18: Appeal Denials Within Timeframes
Insurance carriers impose strict deadlines for filing appeals, often as short as 30 to 60 days from denial notice. Create an appeal calendar that ensures you never miss these critical deadlines. Document your appeal process thoroughly, including dates of contact with payers, representative names, and information provided. Persistence in appeals often results in overturned denials and recovered revenue.
Solution 19: Invest in Staff Education and Training
Regular training for billing, coding, and front office staff pays dividends in reduced denials. Healthcare regulations, coding guidelines, and payer policies change constantly. Quarterly training sessions keep your team current on requirements and best practices. Consider certification programs that demonstrate expertise and commitment to excellence in revenue cycle management.
Solution 20: Partner With Expert Billing Specialists
Sometimes the most effective solution involves recognizing when specialized expertise will serve your practice better than handling billing internally. Professional medical billing services bring deep knowledge of payer requirements, coding expertise, and dedicated denial management resources that most practices cannot match. These specialists often achieve clean claims rates above 95%, dramatically improving cash flow and reducing administrative burden.
Measuring Your Denial Management Success
Track key performance indicators that reveal whether your denial management strategies are working. Your denial rate should remain below 5% of claims submitted. Days in accounts receivable should steadily decrease as you resolve denials faster. Clean claims rate, the percentage of claims paid on first submission, should exceed 90% with effective denial prevention systems in place.
Monitor these metrics monthly and celebrate improvements with your team. When denial rates drop and cash flow improves, everyone benefits from the reduced stress and increased financial stability.
Taking Action to Transform Your Revenue Cycle
Implementing these 20 claim denial management solutions requires commitment, but the financial rewards justify the effort. Start by assessing your current denial rate and identifying your top three denial reasons. Focus your initial efforts on these high impact areas where improvements will generate the most significant results.
Remember that denial management is not a one time project but an ongoing process of continuous improvement. As you master one solution, move to the next until you have built a comprehensive system that prevents most denials and resolves the rest quickly.
Your practice deserves the financial stability that comes from effective denial management. The strategies outlined here have helped countless healthcare practices reduce denials, accelerate cash flow, and reclaim time that staff were spending on rework. Whether you choose to implement these solutions internally or partner with experienced medical billing services, taking action now will protect your revenue and strengthen your practice for years to come.
If you operate in Florida, specialized medical billing services Florida providers understand state specific payer requirements and can accelerate your results. For practices seeking comprehensive support, revenue cycle management services in Florida offer end to end solutions that address every aspect of your billing operation.
Specialty practices face unique challenges that require targeted expertise. Cardiology billing services address the complex coding and documentation requirements specific to cardiac care. Meanwhile, Practice Management Consulting helps practices optimize workflows beyond just billing to improve overall operational efficiency.
When evaluating medical billing companies in Florida or any medical billing company, look for partners who demonstrate expertise in denial prevention, not just denial management. The best services focus on getting claims right the first time rather than fixing problems after they occur.





